This month, we dive deep into hip dysplasia (HD). It’s one of the most commonly diagnosed orthopaedic conditions in dogs, but I know the decision-making process, especially relating to surgery, can be confusing. HD can result in a wide spectrum of clinical signs, from those dogs that are seemingly unaffected by their hips to dogs with severe and chronic hip pain that significantly impacts the quality of life. Most dogs will be managed medically, but there are several surgical options for dogs (and also cats). So what are they, and when do we consider them?
We can split surgical options into two categories: those that are considered ‘prophylactic’ and those that are ‘salvage’ surgeries.
Prophylactic surgeries
1. Juvenile pubic symphysiodesis
Juvenile pubic symphysiodesis (JPS) is the surgical fusion of the pubic symphysis in young puppies such that continued growth of the pelvis results in ventrolateral rotation of each acetabulum and improved ‘capture’ of a dysplastic hip. This is usually achieved by electrosurgery ablation of the symphysis. It is a simple and quick procedure with minimal aftercare requirements. The limiting factor for widespread use of JPS is that it should be performed in puppies between 12 and 16 weeks of age (up to 22 weeks in giant breeds) to be effective. These puppies will not be symptomatic at this age, and so unless at-risk puppies are proactively screened at a young age, they will miss the window of opportunity for the procedure. Screening itself is also problematic. At such a young age, conventional radiographic screening may not identify hip dysplasia. On the VD hip radiograph, extension of a dysplastic (loose) hip can result in tightening of the joint capsule and medialisation of the femoral head into the acetabulum, thus giving the appearance of a normal hip. We will, therefore, generally rely on manual tests such as the Ortolani sign (click for video) to identify hip laxity and thus screen for JPS candidates. With appropriate case selection, JPS can be an effective technique to improve the stability of a dysplastic hip and mitigate the progression of osteoarthritis (OA), and screening is probably sensible for puppies of at-risk breeds (especially if the parent hip scores are poor or unknown) and/or those with a history of hip dysplasia in close family relatives.
2. Triple/Double Pelvic Osteotomy
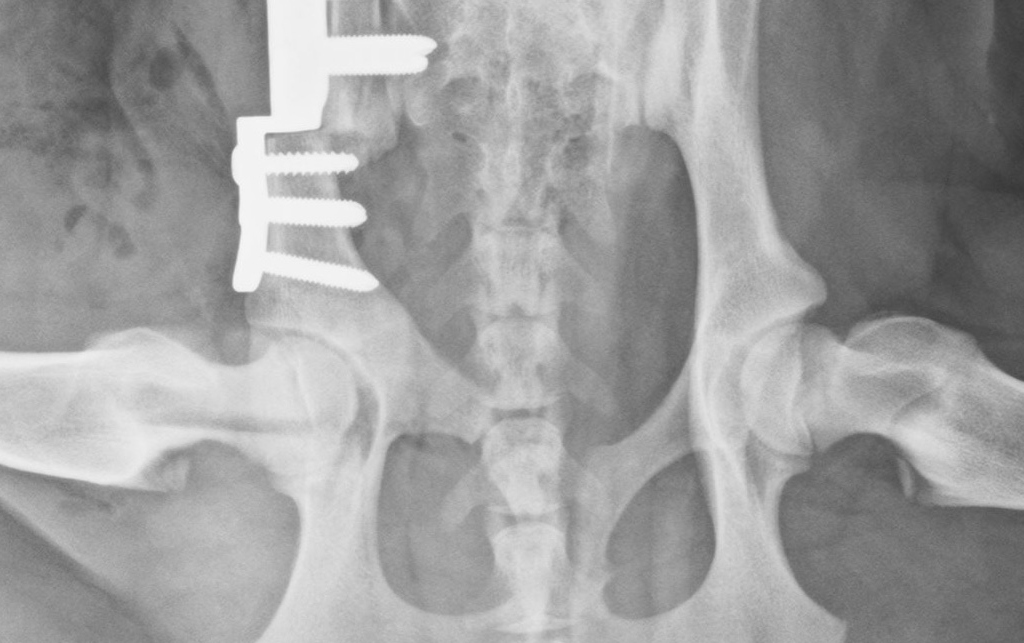
Triple pelvic osteotomy (TPO) involves osteotomies of the ilium, the pubis and the ischium which allow the acetabulum to be rotated ventrolaterally to improve femoral head capture. The rotated bone segment is stabilised with a specialist bone plate on the ilium. TPO has been largely superseded by double pelvic osteotomy (DPO), which is very similar but does not include the ischial osteotomy (and thus does not destabilise the acetabular segment as much as TPO). Both techniques require careful case selection to be effective. They should be performed before the development of secondary osseous changes affecting the hip, and this limits their use to juvenile dogs. Most candidates are 5-10 months of age but this is not a hard and fast rule.
TPO and DPO are major orthopaedic procedures with a risk of potentially serious complications. I will, therefore, reserve these surgeries for dogs with significant hip pain/lameness. Others however will argue that the surgery is justified in non-symptomatic dogs in order to avoid OA. The latter approach does mean that some dogs that will never suffer from their hip dysplasia will be operated on (this is also true of JPS, but JPS is a much less invasive procedure with a very low risk of complications). The potential impact of major orthopaedic surgery at such a young age, with the necessary exercise restriction and impact on behavioural training and socialisation, should also be considered.
TPO and DPO are not often performed in specialist practice in the UK, because of the limitations above. Those of us who reserve surgery for puppies with significant clinical signs find that by the time hip dysplasia has been diagnosed, secondary osseous changes are often already present in the hip. Furthermore, given that total hip replacement (THR) has become a very predictable and successful surgery, puppies with mildly symptomatic hip dysplasia will often be managed non-surgically in the first instance with a view to THR at a later date if there is a persistent clinical issue.

Salvage surgeries
1. Femoral head and neck excision
We are all familiar with femoral head and neck excision (FHNE). It can be a very useful procedure for patients with severe hip pain, especially smaller patients and if financial circumstances mean that THR is not an option. The aim of FHNE is to prevent hip pain by eliminating contact between the acetabulum and the femoral head. Removal of the femoral head and neck results in the formation of a fibrous pseudoarthrosis that, along with the surrounding muscles, supports the hip in the absence of a direct articulation.
FHNE can be a very effective surgery, generally more so for smaller patients. It is often stated that dogs less than 15-20 kg do better than larger dogs, but some larger dogs will also do well after FHNE. The concern with FHNE is that the fibrous pseudoarthrosis that forms can restrict hip mobility and result in persistent hip pain. To minimise the impact of this, all patients should have physical therapy/hydrotherapy after FHNE, and this is particularly important for larger patients, for whom a proactive rehabilitation programme is critical for a good outcome. Return to maximal function after FHNE can take as long as six months.
The outcome following FHNE is unpredictable. Progressive muscle atrophy, restrictive hip mobility and proximal migration of the femur can be seen after surgery. Most owners are satisfied with the outcome after FHNE but may not recognise that their pet has an altered gait. One study looked at the outcome of FHNE in cats and dogs (with the majority being less than 15 kg), using a client questionnaire as well as objective data (kinetic and kinematic gait analysis), and reported good functional results in 38% of patients, satisfactory results in 20% and unsatisfactory results in 42%.
FHNE is very applicable to general practice, but there are some important points to consider. Firstly, make sure that your diagnosis is correct. It is not uncommon for other conditions of the hindlimb, especially cruciate disease, to be falsely attributed to the hip. Secondly, patients with very mild/intermittent clinical signs, especially those that respond well to medication, are not likely to be good candidates for FHNE, given that patients can have persistent hip pain/lameness after FHNE. Finally, pay close attention to surgical technique. Tenotomy of the deep gluteal muscle, which is sometimes part of an approach to the hip, must be avoided so as to not further destabilise the hip. The position of the osteotomy is important to avoid bone spurs that may impinge on the acetabulum after surgery. The osteotomy is ideally performed with an oscillating saw. This is safer and more accurate than other methods. With care, an osteotome and mallet can be used, but these risk fracture of the femur if the bone is brittle or if the cut is directed in the wrong direction. A chisel (which is bevelled on only one side of the cutting edge) should never be used; this is much more likely to result in femoral fracture.
2. Total Hip Replacement
THR has been performed in dogs for more than 40 years, and I’ve been performing them for over 20 years (yikes!). THR systems continue to evolve and improve, and in the right hands, THR is a very predictable technique with good outcomes. I’ve already discussed some of the intricacies of the different THR systems in a previous blog (https://mooresortho.com/blog/total-hip-replacement/), so I won’t repeat myself here.
Femoral Head and Neck Excision vs Total Hip Replacement
The biggest change in THR use over the past 15 years has been the development of a cemented THR system for smaller patients. This has allowed even very small dogs and cats to benefit from THR. These smaller patients can do very well after THR, and THR should be considered as an alternative option for any patient requiring FHNE. Often, these smaller patients will have conditions other than hip dysplasia. Slipped capital femoral epiphyses are the most common indication in cats, and Legg-Perthes disease is a common indication in small dogs. As a further exciting development for the smaller patients, we can now offer mini cementless THR. You might take the view that small patients do well after FHNE, so THR is not necessary. The data cited above suggests that not every small patient does well after FHNE and my personal experience supports this. I performed a THR on my own cat, a crazy Bengal, many years ago (he had hip dysplasia). After several years of running up and down trees, he wore through his cup. Of course, he’s the only cat I have seen do this, having performed multiple feline THRs! I removed the implants, which effectively left him with an FHNE, and he was never as good on that leg as he was with the THR. (Addendum Dec 2024: further research has just been published from the University of Vienna which shows cats have better limb function and are more active after THR compared to FHNE).


Compared to FHNE, THR is more likely to return a patient to full function without pain. However, it is not the right choice for every patient or owner. There is, of course, a big financial difference, although to help with this routine THR at The Moores Orthopaedic Clinic starts at a very competitive £7200 fixed-price and is covered by our surgical guarantee. There is also a big difference in aftercare. Strict exercise restriction is required after THR, generally for at least 8 weeks, whereas FHNE patients are encouraged to be active soon after surgery. For some owners, this will sway their treatment choice. Both FHNE and THR can result in complications. After FHNE, the primary concern is poor limb function. After THR, a complication is more likely to require further surgery. Major complications are seen in around 5-10% of THR patients. Most of these can be managed and the hip replacement preserved, but additional surgery may be needed.
Infection can be a devastating complication after THR, since often the implants may need to be removed to resolve the infection. It is, therefore, critical that THR surgery is performed in the right environment and with appropriate precautions to avoid infection. Our theatres at The Moores Orthopaedic Clinic were specifically designed with a HEPA-filtered ventilation system for this very reason, and they meet human orthopaedic theatre standards. Most veterinary hospitals will not have such ventilation (we had to specifically request our veterinary architects to add it into the design of the clinic). As with any highly technical procedure, complication rates tend to reduce with experience, so do ask your prospective THR surgeon how many THRs they have done (I’ve performed hundreds, by the way!).
Assessing young dogs
So, now we know the surgical options, when should you consider getting in touch with us? It might be worth discussing hip dysplasia with owners of at-risk breeds (such as Labradors, German Shepherd Dogs, etc.) at their puppy vaccinations, and if owners might be interested in JPS then consider checking the hips for an Ortolani sign (this is likely to require sedation), or if you prefer we can perform this assessment for you.
Young dogs with lameness localised to the hips should have hip radiographs taken, but importantly, they should be assessed for Ortolani at the same time since radiographs can provide a false-negative result for hip dysplasia in young patients. If hip dysplasia is confirmed and there are no secondary osseous changes, then DPO may be an option, but we are likely to advocate non-surgical management in the first instance unless the puppy is significantly affected by their hips. If you are unsure, though, please get in touch.
Young dogs with relatively severe lameness, which are not candidates for DPO, may be considered for early THR. We generally prefer to delay THR until at least 10 months of age, but in some circumstances, we will perform THR in younger dogs. Dogs with severe hip dysplasia and luxated (luxoid) hips can have severely compromised mobility and are often treated with early THR.
When should surgery be performed?
Dogs older than 10 months of age with clinical signs attributable to hip dysplasia are managed non-surgically in the first instance. This will include exercise modification, NSAIDs and physical therapy (physiotherapy/hydrotherapy). Owners will have different preferences for how long they pursue these strategies before seeking further advice or considering other options, but THR becomes an option for any patient with clinical signs despite these strategies, for dogs requiring long-term medication or long-term exercise restriction to manage their hip dysplasia/OA (since surgery may eliminate the need for medication/exercise restriction) or for dogs having frequent flare-ups of hip pain due to hip OA. Weight management is an important part of the non-surgical management of OA, but patients who are possible THR candidates should not have surgery delayed whilst weight loss is attempted. Such patients will generally be inactive due to their hip disease, and my experience is that significant weight loss can be a very slow process in these patients. It is generally better to improve patient comfort and activity through THR, and the weight loss will then be far easier to achieve.
Because the outcome after FHNE is less predictable than after THR, where THR is not an option for whatever reason, I am more likely to recommend pursuing non-surgical options for longer, reserving FHNE for cases where the hip dysplasia/OA has more of an impact on the patient. These patients will benefit from physiotherapy and hydrotherapy to improve muscle mass, which may help to avoid surgery but will also help improve postoperative recovery if FHNE does prove necessary.
How old is too old?
I am often asked if there is an upper age limit to THR, and the short answer is there isn’t one. As long as the patient is in relatively good health, then THR remains an option. Older patients may be at increased risk of complications, however, partly because remodelling of the hip is likely to be more extreme and also because there may be changes to bone density and healing times as patients get older.
At The Moores Orthopaedic Clinic, we are able to offer all of the surgeries discussed and are very happy to assess hip dysplasia patients of any age. And if we don’t think surgery is the right option, we will certainly say so.
Andy Moores BVSc DSAS(Orth) DipECVS FRCVS
RCVS Specialist in Small Animal Surgery (Orthopaedics)
EBVS European Specialist in Small Animal Surgery
Andy is one of the most experienced and qualified small animal orthopaedic surgeons in the UK. He has been performing total hip replacement in dogs for over 20 years and in cats for over 10 years.